Journal
ISSN 2397-9232
Volume 1 2015
Volume 2 2016
Volume 3 2017
Volume 4 2018
Volume 5 2019
Volume 6 2020
Volume 7 2021
Volume 8 2022
Volume 9 2023
Volume 10 2024
Volume 11 2025
The views expressed in the articles are those of the individual authors and do not necessarily represent the views of PMG
-
Reflective article: Improving Service Efficiency and Quality
READ MORENov
202528 November 2025
-
Reflective article: Improving Service Efficiency and Quality – Issuing a Manual TIS Wheelchair
READ MORENov
202528 November 2025
Physiotherapist
-
Reflective Article: Posture and Mobility - Does Spasticity Even Matter?
READ MORESep
202526 September 2025
Rehabilitation Engineer
-
Reflective article: Wheelchair Skills for Clinicians
READ MORESep
202512 September 2025
Occupational Therapist
-
Training in Assistive Products (TAP): Overview, Key Facts, WHO Response, TAP Implementation & Impact
READ MOREApr
2025
03 April 2025
-
Transport of wheelchair seated passengers
READ MOREDec
2024
04 December 2024
-
Reflective article: Functional Neurological Disorder
READ MOREOct
2024
02 October 2024
Physiotherapist
-
Reflective Article: Innovation processes to meet the needs of people with disabilities
READ MORESep
2024
03 September 2024
-
Reflective Article on: Functional Neurological Disorder
READ MOREAug
2024
21 August 2024
Physiotherapist
-
Transportation of people seated in wheelchairs:
READ MOREDec
2023
11 December 2023
Rehabilitation Engineer
-
Upper Extremity Positioning - The Missing Seating Intervention
READ MORENov
2023
22 November 2023
Occupational Therapist
-
A client-centred, holistic approach to 24-hour postural management
READ MOREOct
2023
31 October 2023
Occupational Therapist
-
PMG Conference Reflections
READ MOREOct
2023
11 October 2023
Physiotherapist
-
Duchenne Muscular Dystrophy: how can we apply learning to a case?
READ MORESep
2023.jpg)
12 September 2023
Occupational Therapist
-
Sustainable wheelchairs in Kenya
READ MOREFeb
2023
07 February 2023
-
Pressure Mapping in Practice - bursar report
READ MOREDec
2022.png)
13 December 2022
Clinical Scientist
-
Reflections on PMG 2022 plenary session: Speed Networking review
READ MORENov
202228 November 2022
Occupational Therapist
-
Looking for the windows of opportunity
READ MORENov
202208 November 2022
Occupational Therapist
-
Seating and Dystonia - are we getting it right?
READ MORESep
202201 September 2022
Physiotherapist
-
Reflecting on "A Tangle of Dreams"
READ MOREAug
202219 August 2022
Physiotherapist
-
Occupational Therapy and Wheelchair Service Provision
READ MOREJul
2022
29 July 2022
-
Dynamic Seating: providing movement for clinical benefit
READ MOREApr
202222 April 2022
-
National Wheelchair Managers’ Forum: Krys Jarvis standing down
READ MOREMar
2022
07 March 2022
Occupational Therapist
-
David Constantine, Founder Director at Motivation, to step down from 1 January 2022
READ MORENov
2021
23 November 2021
-
Long Covid
READ MOREJan
2021
22 January 2021
Occupational Therapist
-
Sacral Obliquity vs Pelvic Obliquity
READ MOREJan
2021.jpg)
04 January 2021
Occupational Therapist
-
Research review: "Accepting Wheelchair Use" by Linda Walker
READ MORENov
2020
17 November 2020
-
The Science of Seating
READ MOREOct
2020.jpg)
06 October 2020
-
Meeting stability and other seating goals on wheelchair cushions
READ MOREJun
2020
15 June 2020
Occupational Therapist
-
Transportation of people seated in wheelchairs - best practice
READ MOREJan
2020
30 January 2020
Occupational Therapist
-
Integrated access
READ MOREJan
2020.jpg)
16 January 2020
Neuro-physiotherapist
-
Additive manufacturing for the provision of custom-made head supports
READ MOREJan
2020
02 January 2020
Rehabilitation Engineer
-
Influence of tilt-in-space and recline on ischial blood flow and pressure
READ MOREDec
2019
19 December 2019
Occupational Therapist
-
Standing in the wings
READ MOREDec
2019
05 December 2019
Occupational Therapist
-
Beginning power mobility in British Columbia
READ MORENov
2019
21 November 2019
Occupational Therapist
-
Feeling Hot Hot Hot! Can ventilation improve posture?
READ MORENov
2019
07 November 2019
Physiotherapist
-
Parents of adults with multiple sclerosis
READ MOREOct
2019
24 October 2019
Physiotherapist
-
Low cost cushion for pressure ulcers
READ MOREOct
2019
10 October 2019
Trainee Clinical Scientist
-
ISWP Basic Wheelchair Training
READ MORESep
2019
26 September 2019
Occupational Therapist
-
Disrupt disability
READ MORESep
2019
13 September 2019
Occupational Therapist
-
Improving mobility for spinal cord injury
READ MOREAug
2019
29 August 2019
Occupational Therapist
-
A psychologist’s journey into occupational therapy
READ MOREAug
2019
01 August 2019
-
Physical Management for Neurological Conditions, 4th Edition
READ MOREJun
2019.jpg)
17 June 2019
Occupational Therapist
-
Outcome Measures
READ MOREJun
2019
03 June 2019
Occupational Therapist
-
Achieving the optimal set up on ultralight wheelchairs
READ MOREMay
2019
23 May 2019
Occupational Therapist
-
Anatomy and Human Movement
READ MOREMay
2019
09 May 2019
Occupational Therapist
-
One Child One Chair
READ MOREApr
2019.jpg)
15 April 2019
Occupational Therapist
-
The interdisciplinarity of seating: a review
READ MOREMar
2019
29 March 2019
Occupational Therapist
-
Clinical Reasoning in the Health Professions 4th Ed
READ MOREMar
2019
14 March 2019
Occupational Therapist
-
Postural support in lying
READ MOREFeb
2019
21 February 2019
Neuro-physiotherapist
-
Adverse incident reporting and the MHRA
READ MOREFeb
2019.png)
01 February 2019
-
The Stroke Survival Guide by Mark Greener
READ MOREJan
2019.jpg)
10 January 2019
Trainee Rehabilitation Engineer
-
Selective dorsal rhizotomy (SDR)
READ MOREDec
2018
20 December 2018
Trainee Rehabilitation Engineer
-
Cell transplantation research in HD and PD
READ MOREDec
2018
06 December 2018
Rehabilitation Engineer
-
PMG Exhibition 2018
READ MORENov
2018
26 November 2018
Physiotherapist
-
The Comprehensive Textbook of Clinical Biomechanics by Jim Richards
READ MORENov
2018
12 November 2018
Rehabilitation Engineer
-
International Society of Wheelchair Professionals: Basic Training
READ MOREOct
2018
29 October 2018
Occupational Therapist
-
The Reagiro manual wheelchair
READ MOREOct
2018
18 October 2018
Occupational Therapist
-
Becoming differently disabled and learning to listen to the experts
READ MOREOct
201802 October 2018
-
Driving to Learn
READ MORESep
2018
13 September 2018
Occupational Therapist
-
Customised seating
READ MOREAug
2018
23 August 2018
Occupational Therapist
-
Psychologically Informed Physiotherapy
READ MOREJun
2018
25 June 2018
Physiotherapist
-
Creating Capsulá: Promoting Communication in Mexico
READ MOREJun
2018
13 June 2018
-
Wheelchairs and Volcanoes
READ MOREMay
2018.jpg)
24 May 2018
Occupational Therapist
-
Seating and Wheeled Mobility, a Clinical Resource Guide. Ed Michelle L. Lange and Jean L. Minkel
READ MOREApr
2018
26 April 2018
Physiotherapist
-
Shared decision-making and Personal Wheelchair Budgets
READ MOREApr
2018
11 April 2018
Occupational Therapist
-
Book Review: Campbell’s Physical Therapy for Children
READ MOREMar
201829 March 2018
Neuro-physiotherapist
-
Clinical science innovation: is your performance affected by stability?
READ MOREMar
2018
15 March 2018
Clinical Scientist
-
Mobile app technologies in pressure ulcer care and other technological advances at PMG 2017
READ MOREMar
2018
01 March 2018
Occupational Therapist
-
WHO Wheelchair Service Training
READ MOREFeb
2018
15 February 2018
Physiotherapist
-
The Brain Injury Rehabilitation Workbook by Rachel Winson, Barbara A Wilson and Andrew Bateman
READ MOREJan
2018.jpg)
31 January 2018
Occupational Therapist
-
PMG Conference 2017 - a reboot!
READ MOREJan
2018
18 January 2018
Physiotherapist
-
Achieving a person-centred approach to wheelchair seating
READ MOREJan
2018
04 January 2018
Occupational Therapist
-
Complex seating - solving some puzzles at PMG 2017
READ MOREDec
201721 December 2017
Rehabilitation Engineer
-
The Health Gap by Michael Marmot
READ MOREDec
2017
07 December 2017
Clinical Scientist
-
PMG Conference 2017: inspiration, motivation and lots of information!
READ MORENov
201723 November 2017
Rehabilitation Engineer
-
Using wheelchair-controlled video games to provide physically active play for young wheelchair users
READ MORENov
2017
09 November 2017
-
PMG Conference: new technologies and multiple solutions
READ MOREOct
2017
26 October 2017
Occupational Therapist
-
Approaching Disability: Critical Issues and perspectives. By Rebecca Mallett, Katherine Runswick-Cole
READ MOREOct
2017
12 October 2017
Occupational Therapist
-
24-hour Postural Care
READ MORESep
2017
28 September 2017
Occupational Therapist
-
Pressure care and 24-hour postural management
READ MORESep
2017
14 September 2017
Occupational Therapist
-
PMG Conference 2017 - both challenging and welcoming
READ MOREAug
2017
31 August 2017
Occupational Therapist
-
Developing a specialist role in postural management in Rotherham
READ MOREAug
2017
17 August 2017
Occupational Therapist
-
Wheelchair workout
READ MOREJun
2017
21 June 2017
Rehabilitation Engineer
-
Michael Mandelstam - Safety, equipment, restraint: mental capacity and human rights
READ MOREApr
2017
27 April 2017
Occupational Therapist
-
Therapy Outcome Measures for Rehabilitation Professionals, 3rd Edition by Pamela Enderby and Alexandra John
READ MOREApr
2017
20 April 2017
Occupational Therapist
-
PTSD and referring onwards
READ MOREApr
2017
13 April 2017
Physiotherapist
-
Wheels for the World - Uganda, via PMG Conference 2016!
READ MOREApr
2017
06 April 2017
Physiotherapist
-
Paralympic Games in Rio
READ MOREMar
2017
30 March 2017
-
PMG: an eye-opening experience!
READ MOREMar
2017
22 March 2017
PhD student
-
EPUAP; Postural management & surgery
READ MOREMar
2017
16 March 2017
Physiotherapist
-
Post-polio syndrome; International Society of Wheelchair Professionals; Biomechanics of Pressure Ulcers
READ MOREMar
2017
09 March 2017
Physiotherapist
-
Learning the ropes: pressure management, 3D printing, WHO training packages
READ MOREMar
2017
02 March 2017
Physiotherapist
-
Innovation, Outcome measures, Patient-centred care
READ MOREFeb
201723 February 2017
Physiotherapist
-
Mind blowing!
READ MOREFeb
2017
16 February 2017
Occupational Therapist
-
PMG Newbie
READ MOREFeb
2017
09 February 2017
Physiotherapist
-
Musculoskeletal Physical Examination: an Evidence-Based Approach Second Edition
READ MOREFeb
2017
02 February 2017
Specialist Registrar
-
World Health Organisation training packages, critical appraisal, postural correction and more
READ MOREJan
2017
26 January 2017
Rehabilitation Engineer Technician
-
Practicalities of Integrating Assistive Technology
READ MOREJan
2017
19 January 2017
Director
-
PMG Conference 2016: Communication aids, environmental controls and other hot topics!
READ MOREJan
2017
13 January 2017
Trainee Clinical Engineer
-
Joint funded seating
READ MOREJan
2017
05 January 2017
Occupational Therapist
-
Working with augmentative and alternative communication services
READ MOREDec
2016
22 December 2016
Director
-
BHTA honours Barend ter Haar
READ MOREDec
2016
15 December 2016
-
Reflections on collaborative working
READ MOREDec
2016
08 December 2016
Occupational Therapist
-
3D Printing
READ MORENov
201630 November 2016
Supervisor
-
PMG Conference 2016: an invaluable experience
READ MORENov
2016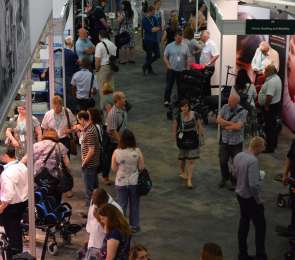
24 November 2016
Physiotherapist
-
PMG Conference: a one stop shop!
READ MORENov
2016
17 November 2016
Rehabilitation Engineer
-
The power of networking
READ MORENov
201610 November 2016
Occupational Therapist
-
Why trainees should attend conferences
READ MORENov
201603 November 2016
Trainee Clinical Scientist
-
Powered wheelchair provision for adults diagnosed with rapidly deteriorating MND
READ MOREOct
2016
27 October 2016
Occupational Therapist
-
Informing clinical practice: reflection on attendance at PMG Conference 2016
READ MOREOct
2016
24 October 2016
Occupational Therapist
-
Braddom's Physical Medicine and Rehabilitation, 5th Edition by David X. Cifu MD
READ MOREOct
2016
13 October 2016
Clinical Scientist
-
Knowledge on postural care amongst nursing students at Birmingham City University
READ MOREOct
2016
06 October 2016
-
Reflections on Personalising Wheelchair Services
READ MORESep
201629 September 2016
Occupational Therapist
-
PMG Conference 2016 - how it's benefiting Devon
READ MORESep
2016
12 September 2016
Occupational Therapist
-
Why "Aldersea" lecture?
READ MORESep
201607 September 2016
-
PMG Conference 2016: A Special Journey
READ MORESep
201601 September 2016
Trainee Rehabilitation Engineer
-
Joining PMG - reaping the benefits
READ MOREAug
201624 August 2016
Occupational Therapist
-
A reflection on the impact of attending the PMG Conference
READ MOREAug
201619 August 2016
Director
-
Making a Difference
READ MOREAug
201611 August 2016
-
PMG 2016 - Inspiring, informative, thought provoking
READ MOREAug
201608 August 2016
Occupational Therapist
-
The code of practice for wheelchair passport schemes – results of a survey of managers
READ MOREApr
2016
18 April 2016
Clinical Scientist
-
Ready to help
READ MOREMar
2016
30 March 2016
Rehabilitation Engineer
-
Book Review - The Atlas of Surface Palpation
READ MOREJan
2016
27 January 2016
Trainee Clinical Scientist
-
Solving the mystery of why a wheelchair is comfortable in clinic but not at home!
READ MOREJan
2016
27 January 2016
Occupational Therapist
-
Wheelchairs revisited
READ MOREDec
2015
01 December 2015
Occupational Therapist
-
A neurophysiotherapist’s view
READ MOREDec
2015
01 December 2015
Neuro-physiotherapist
-
Beyond the Wheelchair – reflections on static seating needs
READ MORENov
2015
01 November 2015
Occupational Therapist
-
My lucky star is shining!
READ MORENov
2015
01 November 2015
Highly Specialist Physiotherapist
-
The journey of a thousand miles
READ MORENov
2015
01 November 2015
Occupational Therapist
-
Eager to Learn
READ MOREOct
2015
01 October 2015
Trainee Rehabilitation Engineer
-
From finding my feet to finding solutions
READ MOREOct
2015
01 October 2015
Physiotherapist
-
PMG - "Event of the Year!"
READ MOREOct
2015
01 October 2015
Rehabilitation Engineer
-
PMG's Impact on Malta
READ MOREOct
2015
01 October 2015
Physiotherapist
-
PMG shaping wheelchair skills training
READ MOREOct
2015
01 October 2015
Occupational Therapist
-
Reflections on the provision of powered wheelchairs
READ MOREOct
2015
01 October 2015
Occupational Therapist
-
Sleep Systems in Hounslow
READ MOREOct
2015
01 October 2015
Specialist Occupational Therapist
-
From Paddling Pools to Posture - Getting up to speed with the PMG Conference 2015
READ MOREAug
2015
01 August 2015
Trainee Clinical Engineer
-
PMG 2015: a thumbnail sketch
READ MOREAug
2015
01 August 2015
Occupational Therapist
-
CPD and Accreditation
READ MOREMar
2015
01 March 2015
Occupational Therapist
-
CECOPS - WHAT IT IS AND HOW IT WORKS
READ MOREJan
2015
01 January 2015
Director
-
CECOPS a personal view
READ MOREJan
2015
01 January 2015
Director






.jpg)


